Watch as primordial neural cells dance across, grow into, and even move 3D scaffolds engineered to heal brain injury from stroke and other trauma. Decorating the scaffold with various nutrients and biochemical signals allow researchers to control what types of brain tissues they become. Credit: Katrina Wilson and Ken Kingery, Duke University.
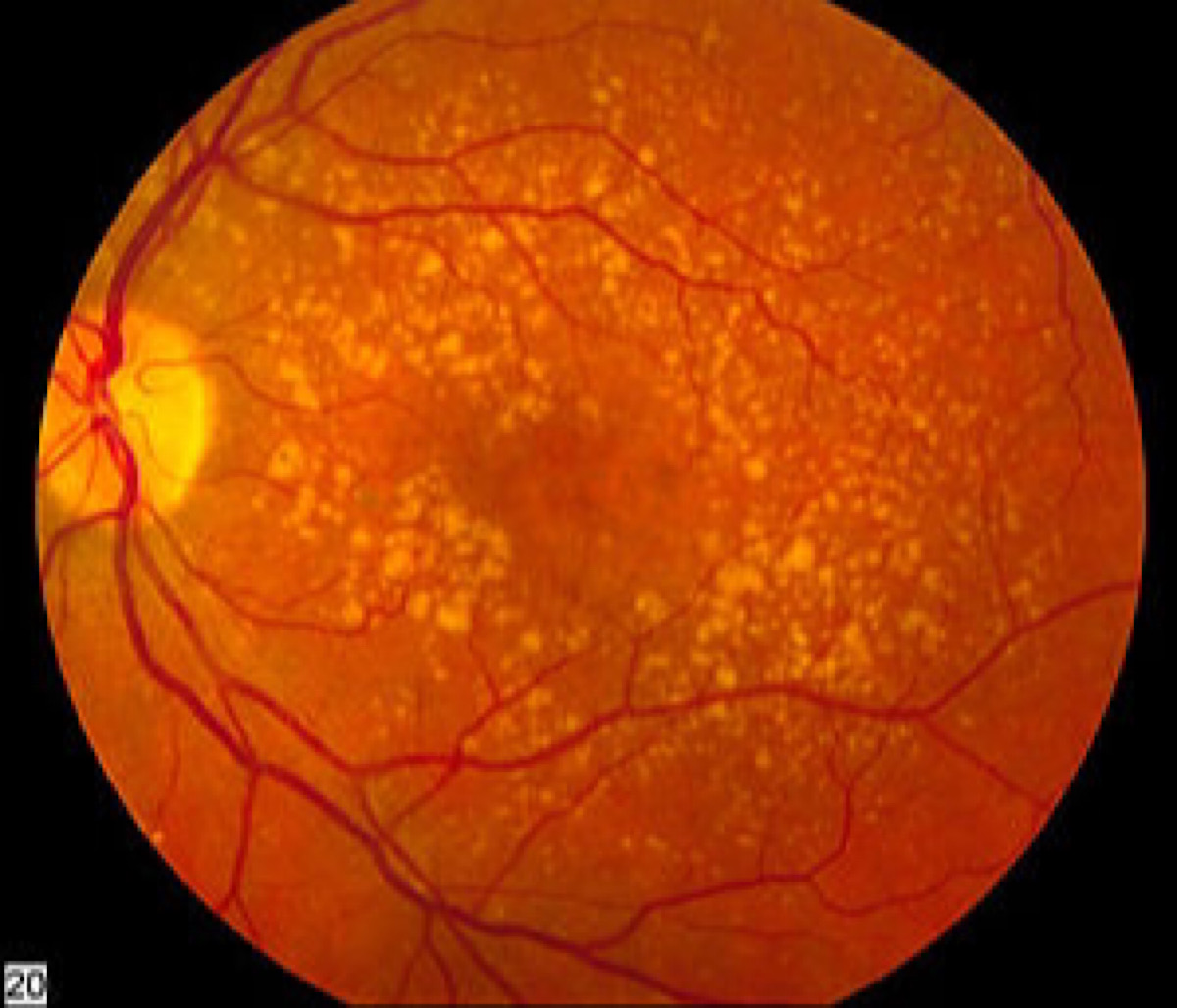
Researchers at Duke University have captured days-long time-lapse videos of young neural cells moving and growing within a novel 3D synthetic biocompatible structure. By literally watching how the cells respond to natural biochemical signals embedded within the material, biomedical engineers hope to develop biogels that can repair and regrow brain tissue after a stroke or other trauma.
The results appear online June 22 in the journal Advanced Materials.
Repairing and regrowing brain tissue is a difficult task. Left to its own devices, the brain does not regenerate lost synapses, blood vessels or other structures after suffering an injury, such as from a stroke. Dead brain tissue is instead absorbed, leaving behind a cavity devoid of anything recognizable as healthy brain tissue.
But that hasn’t stopped researchers from trying to regenerate damaged brains anyway. One common approach used by biomedical engineers is to provide a new medium for the diverse pieces of brain tissue to move into, loaded with various nutrients and biological instructions to encourage growth.
While scientists in the field have historically reached for a homogenous, gelatinous biomaterial to support neural regrowth, Tatiana Segura, professor of biomedical engineering at Duke University, has developed a different approach. Her biomaterial built to encourage all types of healing and growth is made of millions of tiny gelatinous spheres packed together to form a stable scaffold.
Continue reading… “Time-Lapse Footage Shows Neural Stem Cells Grow in 3D Scaffolds”