A new biomaterial scaffold, designed to slowly release stem cells, has worked to ensure implanted stem cells can stick around to relieve pain and reverse arthritis in mice knee joints.
This treatment reduces the quantity of stem cells needed by 90%, thus avoiding the problems of redness, swelling and scar tissue that can arise from large doses of such stem cells. In the near future, it could potentially lead to reversal of osteoarthritis in humans for the first time.
At present, no treatment is currently available that can reverse the course of osteoarthritis, and the sole options are to try to relieve pain. Stem cell therapy potentially offers hope and has been shown to alienate the disease. However, a ‘goldilocks’ dose of stem cells remains out of reach. Too much of a dose and the subject suffers redness, swelling and scar tissue. Too little and the therapy is only successful for a limited period due to gradual cell loss.
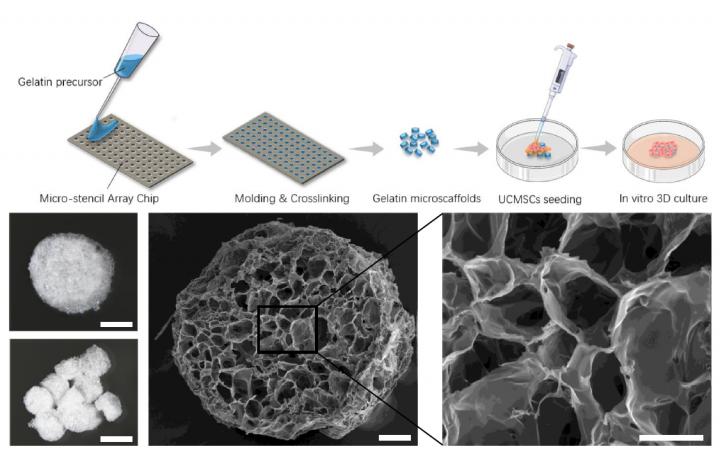
To overcome this challenge, researchers from the Department of Orthopedics at Huazhong University of Science and Technology, China, seeded umbilical cord mesenchymal stem cells on a ‘cryogel’ biomaterial.
Mesenchymal stem cells (MSCs) are adult stem cells that can differentiate themselves into other types of cells. MSCs are sourced from bone marrow, fat, or umbilical cord tissue. Umbilical cord-derived MSCs (UCMSCs) have emerged in recent years as popular therapeutic transplant cells due to their abundant supply, high proliferative capacity, and non-invasive harvesting procedure, and because they pose relatively minor ethical issues.
Cryogels, meanwhile, are gel matrices formed at sub-zero temperatures. They have interconnected macropores (pores larger than 10 micrometres in diameter), much like a sponge. Because these holes can allow mass transport of small particles in them, cryogel biomaterials potentially have a range of biomedical uses.
Credit: Wei Tong, Union Hospital, Huazhong University of Science and Technology
Upon seeding of the stem cells in the cryogel biomaterial, the researchers found that the cells became stronger and showed enhanced therapeutic effects with regard to osteoarthritis in mice. The cryogel also, crucially, ensured the implanted stem cells stayed in the knee joint area for a much longer time. This, in turn, allowed a reduction of the dosage of stem cells by 90%.
“It takes about two weeks for half of the implanted cells to leave, but their regenerative effects stick around for longer,” said Wei Tong, corresponding author on the study, which appears in the Chemical Engineering Journal. “So it is possible that the therapeutic result comes indirectly, via the stem cells secreting epidermal growth factors, which stimulate cell proliferation and healing, rather than directly becoming newly formed cartilage in the joint.”
Tests also showed that the cells were very powerful in reducing joint pain in the mice resulting from inflammation.
Following this proof of concept in mice, the researchers now want to test it out on non-human primates, and then ultimately use the stem cell-cryogel complex in clinical trials on humans, with the hope of developing a new treatment for osteoarthritis that works to reverse the disease.