Every 10 minutes someone is added to the organ transplant waiting list in the US.
As of May 2021, there were over 100,000 people waiting for replacement organs across the country.
And countless more people in need of “spare parts” never even make it onto the waiting list. On average, 17 people die each day while waiting for an organ transplant.
As a result, hundreds of thousands of US deaths could be prevented or postponed with access to organ replacements.
That’s why the recent announcement of the first successful human transplant of an artificial heart in a US patient is such a big development.
The artificial heart used in the transplant was created by medical technology company Carmat, which won FDA approval for human trials just last year. Discussing the latest developments in biotech—using biology as technology—is a key focus of my year-round coaching program Abundance360.
In today’s blog, we’ll discuss how Carmat’s artificial heart works and how it fits into the broader objective of regenerative medicine.
Let’s dive in…
(This article originally appeared on SingularityHub by Vanessa Bates Ramirez, adopted by Peter Diamandis for his Abundance Community.)
ARTIFICIAL HEART SAVES A HUMAN LIFE
Carmat, which is based in France, received approval for its total artificial heart in late 2020.
Now, half a year later, the first US patient has received one of the company’s hearts.
It’s exactly what it sounds like: a heart made of synthetic and biological materials intended for implantation into people who need heart transplants.
The transplant took place last month in a 39-year-old man at Duke University Hospital in North Carolina. The man didn’t go to the hospital expecting to have a heart transplant, but it ended up saving his life.
After experiencing unexpected heart failure, he was diagnosed with advanced coronary artery disease (when plaque builds up in the blood vessels that carry oxygen-rich blood to heart) and went in for bypass surgery (which implants a healthy blood vessel from another part of the body to redirect blood around a blocked artery).
When his condition quickly worsened, his medical team realized bypass surgery wasn’t going to do it, but by that point a traditional heart transplant had become too risky. The patient was in the right place, because not just any transplant center could have implanted an artificial heart.
Carmat got approval from the FDA last year to trial its heart in US patients with end-stage biventricular heart failure, a condition where the chambers that take in and push out blood stop working properly. Duke is one of just three transplant centers in the US participating in the trials, and the surgical team at the hospital had already undergone training for implanting the device.
“You remove the left and right ventricles and then place the artificial heart in its place,” said Dr. Jacob Schroder, an assistant professor in Duke’s surgery department.
He added that the patient was “very stable” throughout the whole process.
HOW EXACTLY DOES CARMAT’S HEART WORK?
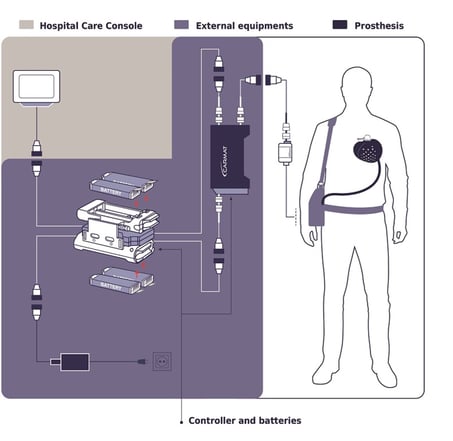
Components of Carmat’s total artificial “robotic” heart. Source: Carmat
The artificial or “robotic” heart has a chamber for hydraulic fluid and one for blood, separated by a membrane. The blood-facing side of the membrane is made of tissue from a cow’s heart, as are the heart’s four valves.
A motorized pump moves hydraulic fluid in and out of the chambers, and that fluid moves the membrane to let blood flow through.
Embedded sensors automatically adapt blood flow to a person’s needs in any given moment. For example, if a person’s exercising, then blood flow will increase.
It’s this aspect that has earned the Carmat heart the designation of “next-generation,” and is what differentiates it from the artificial heart made by American company SynCardia, which is a fixed-rate device, meaning the beats per minute will stay the same regardless of patient activity.
The device weighs 900 grams, or just under 2 pounds (about three times the weight of the average human heart). The external setup is a bit heavier; recipients will have to carry about nine pounds of equipment, including a controller, a bag of actuator fluid, and two battery packs.
In the case of the Duke patient, his artificial heart will stay remotely connected to the hospital’s system so that his doctors can monitor it and be sure it’s functioning as it should.
SO, WHAT HAPPENS NEXT?
Well, just days after the US transplant, a similar transplant took place in Italy, marking Carmat’s first commercial sale of the heart (the difference being that this patient’s transplant was planned, not done as part of a trial or a last resort).
Ongoing trials of the artificial heart will study its use for both temporary purposes—while patients wait for a real heart—and as a long-term solution.
“Many of these patients don’t have a treatment option,” said Dr. Carmelo Milano, chief of adult cardiac surgery at Duke Health, in a virtual press conference. “We believe that this device will…be safer to support patients as a bridge to transplant, but potentially also as a destination treatment.”
FINAL THOUGHTS
The excessive demand for donated organs, not only in the US but globally, will only intensify as technologies like autonomous cars make the world safer, given that many organ donors result from car and motorcycle accidents.
Safer vehicles mean fewer accidents and donations.
Yet organ regeneration and bioprinting represent just one of the three R’s of regenerative medicine: “Replace.”
The other two are Replenish (using stem cells) and Rejuvenate (using young blood and parabiosis).
A dramatic extension of the human healthspan is just over the horizon.
Soon, we’ll all have the regenerative superpowers previously relegated to a handful of animals and comic books.
What new opportunities will open up when anybody, anywhere, and at any time can regenerate, replenish, and replace entire organs and metabolic systems on command?


