Maverick Coltrin was diagnosed with pyridoxine-dependent epilepsy shortly after he was born. He now gets checkups to make sure his seizures are under control and that he’s still healthy. (Kent Nishimura / Los Angeles Times)
Maverick Coltrin entered the world a seemingly healthy 8-pound boy. But within a week, he was having seizures that doctors could neither explain nor control. They warned that he would probably die within a few months.
“I remember my world just came crashing down,” said his mother, Kara Coltrin, 24.
In October, Coltrin and her husband, Michael, began taking hundreds of photos of their son, hooked up to tubes and his skin purplish gray. Family rushed to San Diego from across the country to meet him before he died.
Then, in a last-ditch effort, doctors at Rady Children’s Hospital-San Diego decided to analyze his DNA in case it could reveal what was wrong.
In one of his genes, they found a mutation that had caused a seizure disorder. The attacks could now be controlled with a few medicines.
Today, Maverick is a chubby 6-month-old who bounces on his mom’s knee. He narrows his eyes at strangers, drawing his thick brows together, before easing into a toothless grin.
Maverick benefited from a groundbreaking $25-million federal effort studying the value of sequencing babies’ entire DNA, known as their genome. Doctors in San Diego have shown that genome sequencing can help very sick infants like Maverick.
But the potential to uncover diseases and risks hidden in DNA has sparked a controversial debate: What if all babies had their genomes sequenced?
Other researchers in the same federal project, called Newborn Sequencing in Genomic Medicine and Public Health, have been investigating this broader notion, as well as the sticky ethical questions that come with it.
Using genetics to prevent disease has been envisioned since DNA was discovered more than half a century ago. Ideally, it would flag risks that doctors and parents could try to mitigate, such as a likelihood of obesity or breast cancer. Nowadays, delving into your genetic makeup requires little more than spitting into a tube and mailing away for results.
Yet little is known about how easy access to such information could play out. Many worry about whether parents may treat children differently once they have a window into their future. Researchers also warn that much genetic information isn’t predictive or even accurate, and will undoubtedly lead to anxiety among parents.
“It’s like drinking out of a fire hose,” said Dr. Tracy Trotter, a Bay Area pediatrician and co-chair of the American Academy of Pediatrics’ Council on Genetics. “It’s going to be something people want to do, and when they get the information, they’ll wish they didn’t do it.”
Parents regularly ask Trotter about their child’s 23andMe mail-in genetic tests, detailing their projected risks of lactose intolerance or macular degeneration. Other popular services promise to reveal whether your child will be athletic, overweight or go bald at a young age based on your DNA.
Interpreting babies’ genes could dramatically reshape how people parent and how children grow up. Though the medical community remains doubtful, the dropping costs and availability of genetic testing seems poised to leave skeptics behind.
In a sunlit conference room at UC San Francisco, researchers gathered last spring for their final meeting.
Skepticism filled the room. Each unanswerable question was followed by another.
The 30-person team had a sweeping task: To develop ethics and policy guidelines for sequencing the DNA of every baby born in the United States. The federal project overseeing newborn sequencing research, a five-year effort ending this year, had charged them with exploring such a possibility.
Currently, all babies in the United States have their heel pricked within hours of being born so their blood can be tested for dozens of diseases that could severely harm them if not treated immediately. But making the leap to screening babies’ entire DNA profile wouldn’t help most families and would cost a lot more, experts say.
Much of what a genome test would show cannot be clearly interpreted or acted upon. The San Diego program targets babies who seem likely to be suffering from a genetic condition and may have the most to gain from sequencing. Yet successes such as Maverick are still rare; the researchers have been able to diagnose and treat only a quarter of the children sequenced there.
The Rady program “doesn’t help everybody by a long shot,” said Josephine Johnston, director of research at the Hastings Center, a New York bioethics research institute, and co-lead of the ethics group that met at UC San Francisco.
Genetic science is messy. Many of the 20,000 genes encoded in human DNA remain a mystery to scientists.
Johnston likened widespread genome sequencing to requiring people with no symptoms to undergo an MRI or a CAT scan. The vast majority of what turns up would be meaningless, but might look alarming and prompt unnecessary tests.
“They can cause a lot of worry without really giving any benefit,” she said.
That makes the resulting ethical issues all the more troublesome.
Some fear that if parents learn their child will develop a fatal disease at a young age, it could affect how they treat him. Or what about finding out about a risk of Parkinson’s disease, which typically doesn’t show symptoms until middle age, but has no cure?
There’s an unresolved tension, said Dr. Jonathan Berg, a genetics professor at University of North Carolina School of Medicine, between parents who want to protect their children with this information and children who may not want to ever know it.
Of course, parents regularly make decisions to keep their kids healthy, like giving them vaccines or taking them to get their hearing checked, he said. But imagine not having the option to decide whether to find out if you’ll develop Parkinson’s or Alzheimer’s disease.
“That’s what we have the potential to take away from the future generation,” said Berg, who is also overseeing federally funded newborn sequencing research.
Many genetic tests sold online are already targeted at parents, or even sold as baby shower gifts. One promises to tell you what your baby might look like based on your DNA.
The Boston-based company Veritas Genetics sells entire genome tests for newborns in China for $1,900, and will begin offering the same in the United States in the next two years, said Veritas’ chief marketing officer, Rodrigo Martinez. The company already sells tests for adults in the United States.
“We have a lot of interest and demand,” he said. “Over the next five to 10 years, it will be very clear: Everybody will be sequenced.”
How much does it all cost?
Standard newborn screening in California: roughly $130
Rapid genome sequencing at Rady: roughly $6,000
Genome sequencing from Veritas: $999
23andMe genetic tests: $199
Source: Los Angeles Times reporting
This vision seems to be shared by Dr. Francis Collins, who runs the National Institutes of Health, which is funding the newborn screening research.
In his book “The Language of Life: DNA and the Revolution in Personalized Medicine,” Collins cites the 1997 science fiction movie “Gattaca,” in which parents in the delivery room are told their baby’s chance of developing depression, ADHD and heart failure, as well as a probable age of death.
“Genes are generally not destiny,” wrote Collins, disputing the certainty of some of the predictions. “But a softer version of ‘Gattaca’ may be coming soon.”
Indeed, many expect near ubiquity of genome tests, with the cost expected to eventually drop to $100.
The Food and Drug Administration monitors 23andMe, and last month gave the company the green light to test for the breast cancer gene. But the agency thus far has largely left alone most genetic testing companies, which, like Veritas, require a doctor’s signature. Many experts say there’s often little difference, however, between the companies that require a signature and those that don’t.
Morgan Maeder, 33, learned from a newborn genome test that her daughter Clara was a carrier for polycystic kidney disease. Clara, now 2½, won’t develop the condition herself, but could pass it to her children.
The results prompted Maeder and her husband to get tested to find out which of them carried the mutation and whether their next child could have the disease, she said.
“I would rather just know instead of not knowing,” said Maeder, who lives in Boston.
Dr. Robert C. Green, a medical geneticist at Brigham and Women’s Hospital in Boston who co-directs the sequencing study that Maeder participated in, said he thinks more parents will begin opting for such tests.
“I don’t think we’re actually thinking hard enough about the benefits,” he said.
But when his team visited Boston hospitals, they found that parents weren’t eager to immediately learn every possible detail of their newborns’ genetic profiles. Less than 10% of the thousands of parents they approached agreed to have their babies’ genome sequenced, he said.
Many parents were uncomfortable with the idea of testing, or worried about privacy or discrimination. Though health insurers can’t deny coverage based on potential medical problems identified through genetic testing, life insurance companies can. Another large group of parents were worried, he said, about results that might be frightening or confusing.
Johnston, the ethics researcher, would be in that camp. She’s certain that unclear findings would have stressed her out when her daughter, now 8, was born.
“I’m really glad I didn’t have that temptation to find out a whole bunch of things,” she said. “Newborn babies do weird things — they wave their arms around, they’re cross-eyed half the time — I honestly feel like I would’ve found all of that much more freaky.”
Guidelines due this summer from the bioethics team that met at UC San Francisco will not recommend that genome sequencing become a standard part of newborn screening, said Barbara Koenig, who runs the bioethics program at UC San Francisco and co-leads the team with Johnston.
“There’s been a lot of hype and hyperbole around this idea,” she said. “But it’s going to be quite a while before we actually know whether it’s a good idea to sequence every child at birth.”
All of the federally funded newborn genome sequencing projects wrap up in August and most of the researchers involved are meeting in San Diego this week. Officials from the National Institutes of Health would not say what sort of newborn screening and genomics research would be funded next.
Researchers acknowledge that they ultimately have little control over how these technologies are used, especially as they become widely sold. Some suspect that genetic tests could become a norm of parenting.
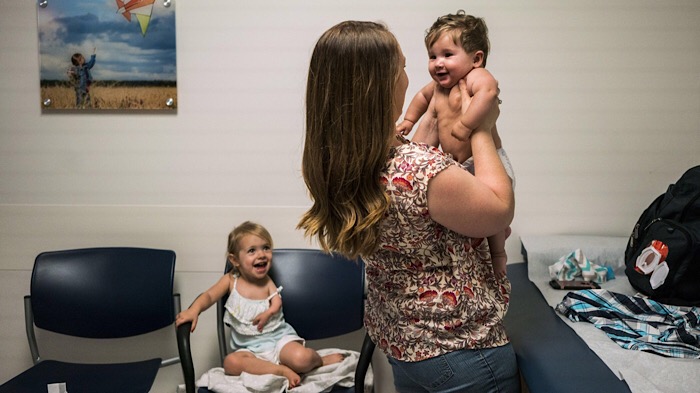
Kara Coltrin, 24, holds up her 6-month-old son, Maverick, during a medical appointment at Rady Children’s Hospital-San Diego earlier this month. Kent Nishimura / Los Angeles Times
On a recent afternoon, Kara Coltrin returned to Rady Children’s Hospital. Maverick sucked on his mother’s thumb as they waited for a doctor’s appointment.
If Kara has another child, she said, she would would want all of the baby’s genetic information, as soon as possible.
“Knowledge is power, right?” she said. “The more knowledge you have, the better you’d be able to take care of them.”
Via LA Times